Spinal Surgery – Guide to Procedures
Introduction: Understanding Spinal Surgery
Common Conditions That May Require Spinal Surgery
Spinal surgery is recommended in specific clinical situations, such as:
1. Herniated Disc
When the soft inner material of a spinal disc protrudes and presses on nearby nerves, it can cause intense pain, weakness, and numbness. Surgical removal of the problematic portion often brings relief.
2. Spinal Stenosis
A condition where the spinal canal narrows, compressing nerves and leading to pain, weakness, or difficulty walking. Surgery can expand the canal and relieve pressure.
3. Degenerative Disc Disease
Age-related wear and tear of spinal discs can cause chronic pain and discomfort. Surgical options aim to stabilize and relieve this pain.
4. Scoliosis and Kyphosis
Abnormal spinal curvature that can worsen over time and impair posture or breathing. Corrective spinal surgery can align the spine and reduce progression.
5. Traumatic Injury
Accidents or falls can damage vertebrae or discs, necessitating surgical intervention for stabilization and nerve decompression.
6. Spinal Tumors
Tumors in or around the spine can compress neural structures and require surgical removal.
7. Spinal Infections & Instability
Certain infections or structural instability from diseases like spondylolisthesis need surgical correction.
Types of Spinal Surgery
Spinal surgery broadly falls into the following categories depending on the condition and desired outcome:
1. Discectomy
A discectomy involves removing a portion of a damaged or herniated disc that is pressing on a nerve root. It can significantly relieve pain and restore mobility. This is one of the most common spinal procedures.
2. Laminectomy and Laminotomy
These decompression surgeries involve removing part of the vertebral bone (lamina) to create more space for spinal nerves. They’re often used to treat spinal stenosis.
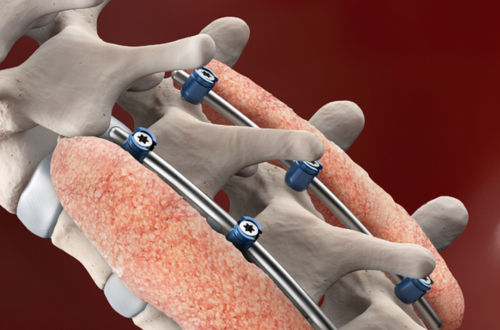
3. Spinal Fusion
Spinal fusion is a stabilizing procedure where two or more vertebrae are fused to prevent painful movement between them. It’s effective for conditions like fractures, scoliosis, and degenerative disc disease.
4. Endoscopic Spine Surgery
This is a minimally invasive technique that uses an endoscope to visualize and treat spinal pathology through small incisions, reducing pain, blood loss, and recovery time.
5. Minimally Invasive Spine Surgery (MISS)
Using small incisions and specialized tools, MISS aims to decrease tissue damage and accelerate recovery. It’s becoming the preferred approach for many spine conditions.
6. Artificial Disc Replacement
Instead of fusing vertebrae, in some cases a damaged disc is replaced with an artificial implant to preserve motion.
7. Vertebroplasty / Kyphoplasty
These procedures treat compression fractures by injecting bone cement into fractured vertebrae to stabilize them and reduce pain.
Who Should Consider Spinal Surgery?
Spinal surgery is often considered when:
Severe pain persists despite non-surgical treatments.
Numbness, weakness, or balance issues worsen.
Nerve compression leads to loss of bowel or bladder control (a medical emergency).
Structural deformity or instability is progressive.
Quality of life is significantly affected and daily activities are compromised.
Eligibility depends on age, overall health, extent of spinal damage, and specific diagnosis. There is no strict age limit — even older adults can benefit when carefully evaluated.
Pre-Operative Evaluation & Preparation
Before surgery, a thorough assessment is conducted:
Detailed medical history and physical exam.
Imaging tests like MRI, CT scan, or X-rays to evaluate spinal structures.
Blood tests and anesthesia evaluation.
Discussion about risks, benefits, expected outcomes, and recovery process.
Ask your spine surgeon important questions such as:
Why is surgery recommended?
What are the alternatives?
What are the risks and benefits?
What is the expected recovery timeline?
The Surgical Procedure
The exact steps vary by the type of surgery, but most share common elements:
Anesthesia: General anesthesia ensures you are pain-free and comfortable.
Incision: The surgeon makes an incision to access the affected spinal area.
Target Procedure: This could involve removing part of a disc, decompressing nerves, stabilizing vertebrae, or implanting hardware.
Closing: After completing the procedure, the incision is closed, and sterile dressings are applied.
Monitoring: Vital signs and neurological status are monitored immediately after surgery.
Minimally invasive techniques use smaller incisions, specialized cameras, and instruments to reduce tissue trauma and hospital stay.
Benefits of Spinal Surgery
The primary goals and benefits include:
Pain Relief: Significant reduction in back or leg pain.
Improved Mobility: Many patients regain function and activity levels.
Stability: Fusion and stabilization procedures restore spinal integrity.
Nerve Decompression: Relieving pressure on spinal nerves can reduce symptoms like numbness and weakness.
Quality of Life: Returning to daily activities and improved sleep.
Recovery and Rehabilitation
Recovery varies by procedure but generally includes:
Hospital Stay
Often 1–3 days for minimally invasive procedures; longer for extensive fusions.
Early Recovery
Pain management with medication.
Light walking is encouraged soon after surgery.
Avoid lifting, bending, or strenuous activity in early weeks.
Physical Therapy
Rehabilitation focuses on strengthening core and back muscles to support healing and improve function.
Return to Work
Depending on job type and procedure, many patients resume light work in 4–6 weeks, with full recovery spanning 3–6 months.
