What Are Spinal Injections?
Advanced Minimally Invasive Spine Treatment by Dr. Alok Gadkari
Spinal injections are procedures in which medications — typically steroids, anesthetics, or biologic agents — are injected near spinal nerves, joints, or discs to reduce pain and inflammation. These procedures are performed with imaging guidance such as fluoroscopy (real-time X-ray) or ultrasound to ensure accurate placement.
Spinal injections serve two primary purposes:
Diagnostic: To identify the specific source of pain.
Therapeutic: To alleviate pain and support recovery.
Common Conditions Treated with Spinal Injections
Spinal injections are effective for multiple spine-related conditions, especially when pain is chronic or nerve-related:
Chronic Back Pain
Sciatica / Radiating Leg Pain
Herniated or Bulging Discs
Spinal Stenosis (Narrowing of Spinal Canal)
Facet Joint Pain & Arthritis
Radiculopathy (Nerve Root Compression)
These injections help reduce inflammation around nerves and joints, allowing patients to engage more effectively in rehabilitation programs.
Types of Spinal Injections
1. Epidural Steroid Injections (ESI)
This is the most common spinal injection. The medication is delivered into the epidural space — the area surrounding the spinal cord and nerve roots. It mainly targets swelling and irritation around nerves.
Used for:
Lumbar (lower back) pain
Cervical (neck) pain
Sciatica
Stenosis
Herniated discs
2. Transforaminal Epidural Steroid Injection (TFESI)
Also called a nerve root block, this injection targets a specific nerve root at its exit point from the spine. It delivers medication more precisely to the irritated nerve.
Used for:
Unilateral radicular pain
Foraminal stenosis
Disc herniations with nerve involvement
3. Caudal Epidural Injections
Given at the base of the spine through the sacral hiatus, this injection covers the lower spine. It’s useful in cases where widespread lumbar nerve soothing is needed.
4. Facet Joint Injections
These target the small joints between vertebrae that can become painful due to arthritis or overuse. The medication reduces inflammation and pain in the joint.
5. Trigger Point Injections
Used for muscular pain (“knots”) near the spine. These injections may include anesthetic and steroid to relax muscle tension.
How Are Spinal Injections Performed?
Spinal injections are outpatient procedures performed by specialists such as interventional pain doctors, neurologists, or spine surgeons. They follow these general steps:
Evaluation & Imaging: Review of medical history and imaging (MRI, CT, X-ray).
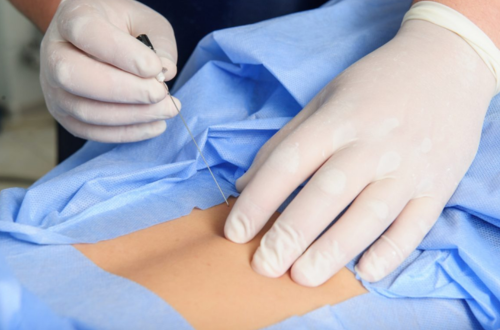
Preparation: The skin is cleaned and local anesthesia is applied.
Guided Injection: A needle is carefully placed using fluoroscopic or ultrasound guidance.
Contrast Dye: In some cases, a contrast dye is injected first to confirm precise placement.
Medication Delivery: Steroids, anesthetics, or biologic agents are injected.
Observation & Recovery: Patients are monitored briefly before going hom
What Medications Are Used?
Medications commonly used in spinal injections include:
Corticosteroids: To reduce inflammation.
Local Anesthetics: For immediate pain relief.
Biologics/Growth Factors: In some protocols, these support healing at the cellular level.
Benefits of Spinal Injections
Spinal injections offer several advantages:
Pain Relief Without Surgery
In many cases, spinal injections can significantly reduce pain without the need for invasive surgery.
Inflammation Reduction
By reducing inflammation near irritated nerves and joints, injections can relieve symptoms and improve function.
Enhanced Rehabilitation
Relief from injections often enables patients to participate more effectively in physical therapy and strengthening exercises, enhancing long-term recovery.
Short Recovery Time
Most patients can return to daily activities within 24–48 hours.
Who Is a Good Candidate?
Ideal candidates for spinal injections:
Patients with chronic pain lasting more than 3 months
People with nerve-related symptoms (e.g., sciatica)
Individuals who have not responded fully to conservative measures
Patients seeking non-surgical pain relief
Who Should Avoid Spinal Injections?
Patients not typically recommended for spinal injections include those with:
Active infection or systemic illness
Bleeding disorders
Uncontrolled diabetes or high blood pressure
Allergy to contrast dye, anesthetic, or steroid medication
Your specialist will assess your medical history and risk factors before recommending injections.
Recovery & Aftercare
After your injection:
Avoid strenuous activities for 24–48 hours.
Monitor for any new or worsening symptoms.
Continue prescribed physical therapy if recommended.
Follow up with your doctor as advised.
Results may vary — some patients feel relief immediately, while others may see improvement over several days.
Spinal Injections vs. Surgery
Spinal injections are often considered before surgical options, especially in cases of moderate pain. The benefits include:
| Feature | Spinal Injections | Surgery |
|---|---|---|
| Invasiveness | Minimally invasive | Highly invasive |
| Recovery Time | Short | Longer |
| Pain Relief | Moderate to strong | Strong (for specific conditions) |
In many cases, injections can delay or even prevent the need for surgery. Your surgeon will guide the best choice based on your condition and imaging findings.
